Bankability: Factors that influence the preservation of your baby’s cord blood
This study looks at factors that can influence cord blood usability to increase the likelihood of banking.
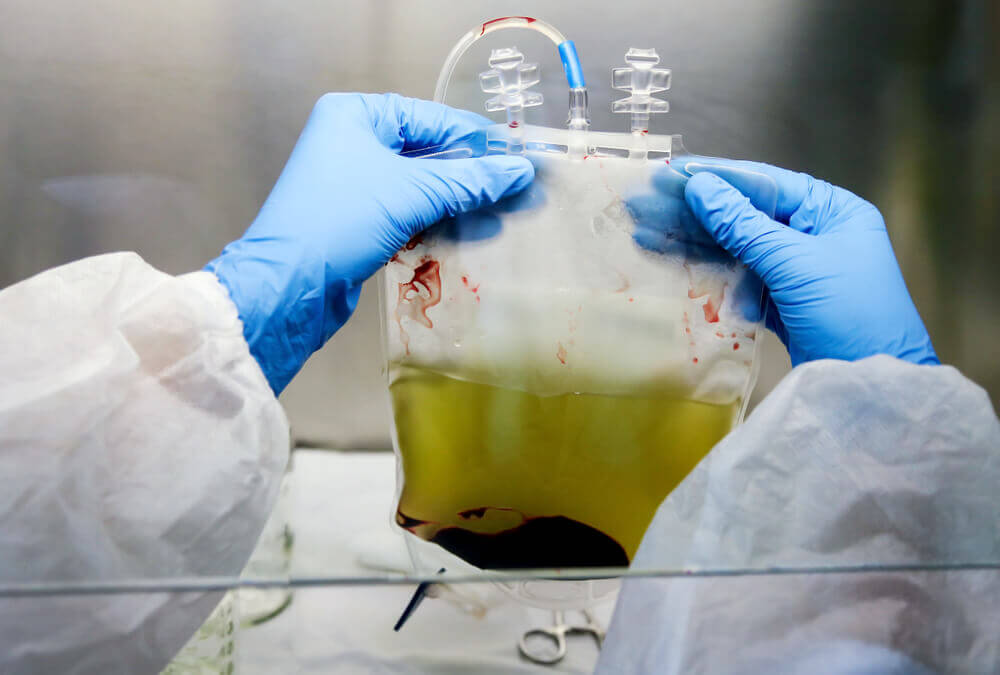
Umbilical cord blood
For centuries, the umbilical cord and the blood left in it (cord blood) were discarded as medical waste. Today, we know that cord blood is one of the richest sources of stem cells, specifically hematopoietic stem cells.
Hematopoietic stem cells are early-stage cells that have the potential to produce all other types of blood cells. They have been used to treat blood-related diseases with stem cell transplants for over 30 years.
Not only that, cord blood stem cells are being explored for their therapeutic potential for treating many other preventable diseases.
Cord blood banking
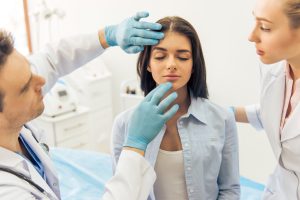
Knowing the benefits, deciding to preserve your baby’s cord blood is easy. And if you do, your doctor will collect the cord blood after the baby is born. The whole process is non-invasive and painless. You do not need to make any special modifications to your birth plan.
What happens when your sample arrives in the lab, on the other hand, is quite complex. It involves separating and collecting stem cells, quality checks to ensure sterility, viability (ability to grow), and sometimes stem cell typing, which looks at markers on the surface of the stem cells used for stem cell matching.
How variability between cord blood samples affect banking
All of the steps involved in collecting, processing, and preserving cord blood are standardized. But this does not mean that there won’t be variation from baby to baby on the amount of cord blood collected, and the number of stem cells in the cord blood sample.
Studies also show that factors like a baby’s birth weight, the size of the placenta, the volume of cord blood collected, and the delivery method (cesarean vs. vaginal delivery) can impact the total number of cells in cord blood samples.
Factors affecting bankability
Sample variability is a problem because low blood volumes and a reduced number of cells can make a percentage of collected samples unsuitable for banking. In this paper, scientists refer to this as ‘bankability’ or the probability of banking, which considers how useful a cord blood sample will be for future use in terms of a transplant or research use.
The study aimed to look at all possible factors that could affect the bankability of a cord blood sample, particularly ones that can be adjusted to increase the likelihood of samples being banked. Some of the factors considered included placental size, weight of the baby, APGAR scores, the amount of liquid infused in to the mother during the delivery, and the delivery method.
Size and delivery method matters
The researchers looked at 869 cord blood samples banked over 15 years, from 1999 to 2015. All babies were born after 35-weeks of gestation, and the cord was clamped 60 seconds after birth. Only samples with a total volume of 91mL (milliliters) were included in the final analysis.
Also, only samples with more than a billion cells were processed and cryopreserved. In agreement with previous research, the the researchers found higher placental weight and vacuum-assisted delivery were linked to an increased likelihood of having more than a billion cells per sample.
They also found a link between bankability and the amount of liquids (e.g. saline solution, blood transfusion) administered to the mother. The bankability decreased by about 30% with each 500mL of liquid infused. It was hypothesized that hemodilution, where the number of cells is diluted or reduced due to an increase in the amount of liquid, may be responsible.
Predicting bankability
The researchers were also able to generate a chart (called a nomogram), which can now be used to predict the bankability of a cord blood sample. The chart is based on the three variables linked to bankability: weight of the placenta, delivery method and how much fluid was given to the mother during labour. As research into this field grows, we can identify more and more external factors that can be managed by delivery teams to increase the likelihood of your baby’s precious stem cells from being preserved.
Reference
Di Tullio, I, Azzolina, D, Niccolò Piras, G et al. (2020). Factors associated with blood cord unit bankability: an analysis of a 15-year-long case series. Cell and tissue bank. 21:77–87. doi: https://doi.org/10.1007/s10561-019-09799-y.
Related Posts
Novel Cord Blood Stem Cell Treatment Leads to HIV Remission

Stem Cell Transplantation Shows Potential in Stroke Recovery