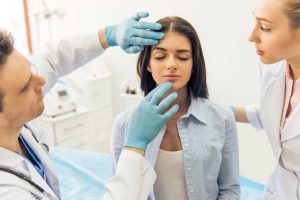
Cell-free therapy using cord tissue stem cells for treating Alzheimer’s disease

Scientists explore the potential of using cord tissue mesenchymal stem cell extracts to slow Alzheimer’s disease progression.
Tackling Alzheimer’s Disease
Alzheimer’s disease and other dementias will affect more than 75 million people around the world by 2030 and 131 million people by 2050. It is a progressive neurodegenerative disease, which means nerve cells are increasingly damaged as the disease progresses. Scientists have identified several different factors like the buildup of protein clumps known as plaques and tangles and the accumulation of toxins, all of which can contribute to Alzheimer’s progression.
Currently, there is no cure for Alzheimer’s. Existing therapies focus on managing symptoms and slowing down progression. There is a need for a therapeutic approach that will prevent or even reverse the nerve damage seen in Alzheimer’s. Researchers in this study aims to develop an Alzheimer’s treatment using cell-free therapy.
Cell-free Therapies
It is well established that stem cells have incredible therapeutic potential, which is why scientists have been looking at them to treat a multitude of diseases including Alzheimer’s. Recent research involving stem cells has focused more on an approach known as cell-free therapy.
Cell-free therapy is based on the idea that rather than using stem cell transplants, we can use stem cells as a source of therapeutic factors or molecules to develop treatment options. Here, the content inside stem cells are removed, and these molecules are delivered to the patient to treat disease.
Several studies show that cell-free therapy may be beneficial for tackling neurological diseases, among others.
Wharton’s Jelly Mesenchymal Stem Cells
Wharton’s jelly is the gelatine-like material that provides insulation and protection to the umbilical cord. It is also a rich source of stem cells known as mesenchymal stem cells (MSC). MSCs have unlimited regenerative potential and act like a medical surveillance team in our bodies, fighting inflammation and activating the immune system, allowing cells to regenerate.
If you choose to preserve your baby’s cord tissue, the Wharton’s Jelly and the MSCS within it will be cryopreserved for later use. Your child will have access this valuable source of stem cells in the future if/when necessary. For example, if scientists develop a cell-free therapy to tackle Alzheimer’s in the future, your baby will have access to a perfectly matched stem cell sample that can be used for this purpose.
The umbilical cord is usually discarded as medical waste. You can choose to save the cord without having to make any changes to your birth plan or affecting your baby’s health in any way.
Wharton’s Jelly Stem Cell Extracts Show Neuroprotective Effects
As mentioned already, cell-free therapy involves removing the material within stem cells. The next step involved packing this content or material into structures called vesicles, which are small fluid-filled sacs for delivery. The first part of this study focused on looking at the feasibility of generating vesicles containing MSC extracts using cells isolated from Wharton’s Jelly. Researchers showed that they can effectively isolate MSCs from Wharton’s jelly and generate vesicles containing their content (hMSC-EVs).
They next went on to study the neuroprotective effects of hMSC-EVs using a hippocampal cell model. Hippocampal cells are derived from a specific region of the brain and serve as a good model for Alzheimer’s. These cells were first exposed to oxidative stress. Oxidative stress leads to cell damage and often the brains of Alzheimer’s patients show this kind of damage. Amazingly, when these cells were provided with hMSC-EVs, the amount of oxidative stress was reduced, highlighting that hMSC-EVs can protect nerve cells from this type of cell damage.
Cord Tissue Mesenchymal Cell-Based Therapies for Alzheimer’s
Findings from this study support the idea that cell-free therapy is a viable option for delivering biomolecules to reduce the disease pathology of Alzheimer’s.
Given that vesicles are able to cross the blood-brain barrier and be administered intravenously, it provides an attractive, alternative treatment option for Alzheimer’s, which needs to be explored further with additional studies.
Reference
Bogart-Santos, V, de Carvalho, LRP, de Godoy, MA. et al. (2019) Extracellular vesicles derived from human Wharton’s jelly mesenchymal stem cells protect hippocampal neurons from oxidative stress and synapse damage induced by amyloid-β oligomers. Stem Cell Res Ther. 20;10(1):332. doi: 10.1186/s13287-019-1432-5.
Related Posts
Novel Cord Blood Stem Cell Treatment Leads to HIV Remission

Stem Cell Transplantation Shows Potential in Stroke Recovery