Healthcord Webinar Series
The immune system and aging
Duration
4:15 minutes
Category
Stem cell therapy
Series
Immunity and aging
Objective
Educational
What you will learn
- What is immunity?
- What happens to your immune system as you age?
- How the age of the immune system influences our susceptibility to COVID-19
- Enhancing our antibody repertoire
- Pandemic flu and the risk of infections
The immune system and aging
In this lesson, we explore immunity, the changes that take place in our immune system with age and how they leave us vulnerable to infections as we age.
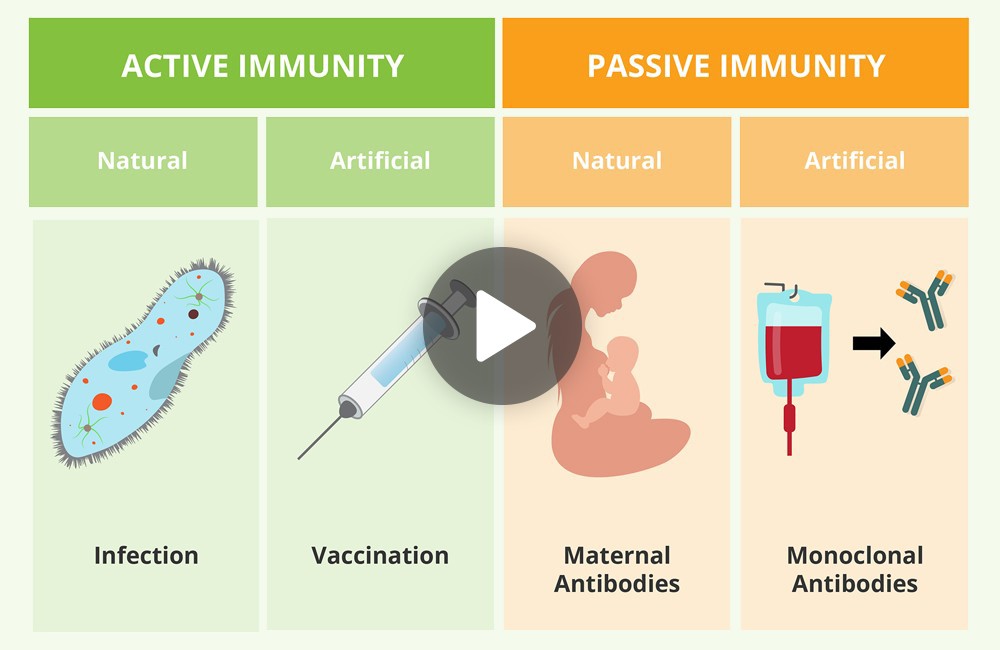
Every day we are exposed to pathogens in the environment. Luckily our immune system can recognize these pathogens and destroy them before they can take over our bodies. As such, acquiring a strong immunity system is key to being able to properly respond to infections.
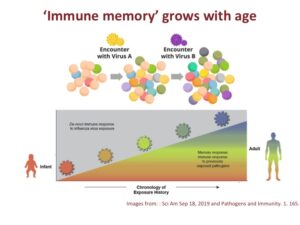 Humans are born with an immature immune system. We build our antibody repertoire or immune memory as we age when we are exposed to different pathogens.
Humans are born with an immature immune system. We build our antibody repertoire or immune memory as we age when we are exposed to different pathogens.Next, you are exposed to virus B. As a result, new antibodies are added to your repertoire to recognize virus B. Your immune system now contains antibodies to recognize both virus A and virus B.
Each instance a person is exposed to a new pathogen, this process is repeated. The end result then is quite simple. Every day, we are exposed to many different microbes in the environment. As a result, our immune systems continue to develop its strength until we start to age.
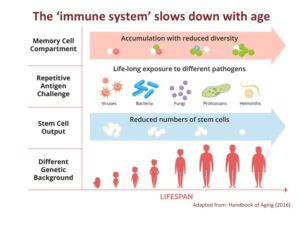 However, this perfect system, is not quite perfect, because our immune systems slow down as we age. While you are most certainly exposed to more pathogens with age, our immune systems change as we age, influencing its ability to protect us.
However, this perfect system, is not quite perfect, because our immune systems slow down as we age. While you are most certainly exposed to more pathogens with age, our immune systems change as we age, influencing its ability to protect us.
As we age, our immune memory is lost. The diversity of the ‘memory’ cells that hold information about antibodies decreases as we age, leading to immune memory loss.
In addition, the stem cell number is reduced with age. Since the hematopoietic stem cells in the bone marrow are responsible for replenishing the immune system, our capacity to replenish cells in the immune system decreases with age.
Finally, changes occur in our DNA with age. These DNA changes can influence the function of stem cells. Studies show that older stem cells are not as robust as young stem cells in terms of their capacity to produce new cells.
Why is immune aging or immune senescence a problem? The following case studies can provide us with much insight into this question.
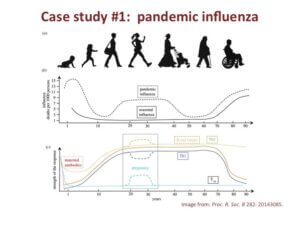 The first study examined pandemic influenza observed a link between the number of influenza deaths and age. The very young and the very old are much more susceptible and are likely to perish from the flu.
The first study examined pandemic influenza observed a link between the number of influenza deaths and age. The very young and the very old are much more susceptible and are likely to perish from the flu.
What’s more, this disease severity corresponds well with the robustness of the immune system and its ability to respond to infections with age. Newborns who have immature immune systems and the elderly with ‘aged’ immune systems are unable to respond to infections with the same robustness of a younger person.
As a result, both the seasonal and pandemic flus are much more dangerous to people in these specific age groups.
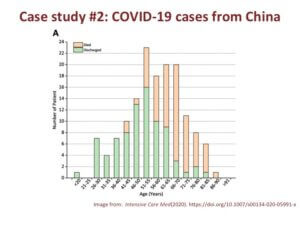 The second study investigated COVID-19 data from China. Similar to the flu, COVID-19 infections were more likely to be lethal to a person over the age of 65.
The second study investigated COVID-19 data from China. Similar to the flu, COVID-19 infections were more likely to be lethal to a person over the age of 65.What is important to realize is that ‘immunosenescence’ or the aging of the immune system can dramatically increase the risk of any infection and its severity as we grow older.
To find out more, visit our lesson highlighting the research that is underway to solve this problem of the aging immune system.
More topics you might like
Continue your journey by selecting another topic.
What are newborn stem cells and why are they important?
3:45 minutes | Stem cell basics
What is immunity and how is it developed?
5:00 minutes | Stem cell therapy
Exploring ways to restore immunity
6:00 minutes | Stem cell therapy
A Precious Gift of a Lifetime
Registering for stem cell banking takes only a few minutes.
A Precious Gift of a Lifetime
Registering for stem cell banking takes only a few minutes.