Viruses, immunity and stem cells
The COVID-19 pandemic has changed the way we see pathogenic infections and their consequences. Keeping with this trend, we wanted to explore the link between infections, immunity, and stem cells in this blog post. Find out more about what happens to our immune system as we age and why cell therapy may be one possible way to mitigate future global pandemics.
What is immunity?
Immunity is the ability our bodies possess for recognizing and disposing of foreign substances such as viruses and bacteria before they can harm us. There are many different layers to the immune system. Two of the main layers are innate immunity and adaptive immunity.
The innate immune system is responsible for the first and immediate response to a pathogen. Components of the innate immune system include physical barriers such as our skin that can stop pathogens from entering the body and white blood cells recruited to identify foreign bodies.
More importantly, perhaps, the innate immune system is responsible for activating the adaptive immune system. This activation is critical because if a pathogen manages to evade the innate immune response, it is necessary to have the adaptive immune system ready to take on the second line of defense.
 Adaptive immunity
Adaptive immunity
Adaptive immunity is more complex and involves producing antibodies. It allows the body to react with a much more robust immune response and creates immune memories necessary for “remembering” pathogens if there is ever a second infection.
We can obtain adaptive immunity passively, meaning through the breast milk of the mother or blood transfusions, or actively via exposure to a pathogen or through vaccination.
In all cases, adaptive immunity involves generating antibodies and immune memories. This immune memory of the adaptive immune system improves with age. Enhanced exposure to pathogens over the lifetime of an individual contributes to growing their antibody repertoire.
The evolution of the immune system
But, the strength of our immune system changes as we age. This aging of the immune system explains why our elderly population is much more vulnerable to infections and why these infections can often become life-threatening.
During the lifetime of an individual, their immune system undergoes many different changes. As babies, we begin with an immature immune system that grows and evolves as we are exposed to pathogens and then declines with age.
This immune decline increases our risk of contracting pathogenic diseases as we age. Infections are still the fourth most common cause of death in the elderly, and they are three times as likely to die from an infection.
In one study, researchers examined the links between age, immunity, and susceptibility to influenza. As expected, the very young and the elderly were much more likely to perish from the seasonal flu or a pandemic flu, which corresponded with their inability to elicit a robust immune response. This link between the elderly and disease lethality also holds for COVID-19.
The aging immune system and stem cells
Studies comparing young and old immune systems have identified many different aspects that change as we age. These changes ultimately contribute to increasing the risk of many other ‘aging’ diseases such as cancer, heart disease, and Alzheimer’s.
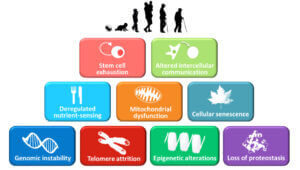
Some of these changes involve changes to our DNA, which impacts the robustness of our immune response, a reduction in immune cell diversity, and, most importantly, perhaps a decrease in the number of stem cells that are important for replenishing the immune system.
Stem cells are early-stage cells that can give rise to other types of cells in the body. Many of the immune cells are generated from one kind of stem cells found in the bone marrow known as hematopoietic stem cells (HSC).
The number of hematopoietic stem cells, and their capacity to replenish cells in the immune system will decrease.
Rejuvenating the immune system with cell therapy
Many scientists believe that hematopoietic stem cells hold the key to restoring the immune system. Consequently, they are exploring the possibility of either reprogramming old stem cells or introducing ‘young’ stem cells into an elderly person with cell therapy.
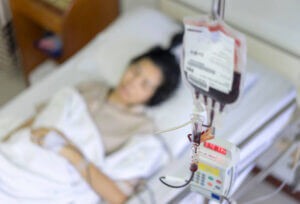
Cell therapy involves introducing living cells into a person through a blood transfusion. Today cell therapy is being used as a treatment option for cancer in a method known as CAR-T cell therapy. CAR-T therapy involves extracting immune cells from a person, engineering them in the lab to recognize cancer cells, and reintroducing them back to the same individual.
With regard to the immune system, scientists are exploring the option of proving older adults with stem cells from younger donors to rejuvenate their immune system.
Cord blood as a source of HSCs
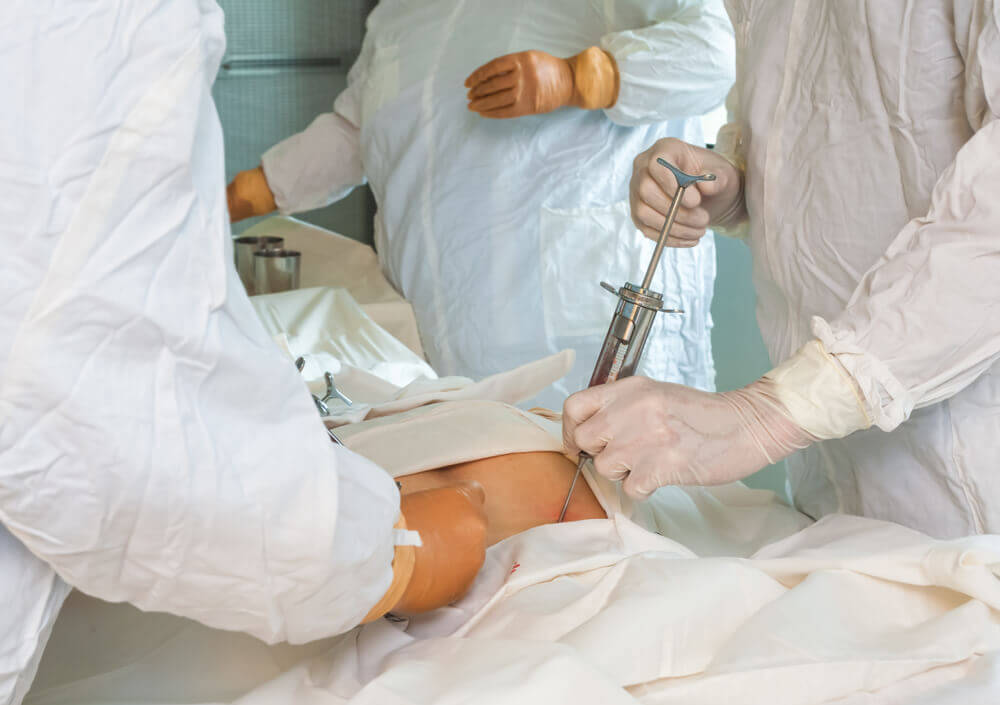
In adults, HSCs are found in the bone marrow, which means donating bone marrow involves surgery, which is why scientists are looking at alternative sources for HSCs such as cord blood.
When a baby is born and the cord is cut, some blood gets left behind in the umbilical cord. This blood is known as cord blood, and it is a valuable source of HSCs. It is possible to collect and preserve these precious stem cells. What’s more, cord blood is collected at birth, which means these stem cells will be at their youngest possible age, without many of the aging markers, stem cells acquire as we age.
Promising evidence
Why do scientists believe cell therapy may be one way to rejuvenate the immune system?
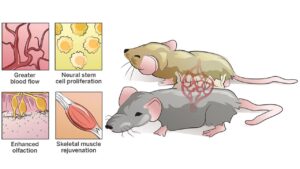 Some of the most promising evidence for this comes from studies in mice. Researchers performed parabiosis experiments where they fused the blood supplies of a young and an old mouse, and then looked at what happened to the cells and tissues of the old mouse after a certain time.
Some of the most promising evidence for this comes from studies in mice. Researchers performed parabiosis experiments where they fused the blood supplies of a young and an old mouse, and then looked at what happened to the cells and tissues of the old mouse after a certain time.
Amazingly they saw the rejuvenation of the cells and tissues of the older mouse in several different systems. In essence, the body of the aging mouse was ‘made young’ following the fusion.
Uncovering the fountain of youth with stem cells?
Immunity is the key to staying healthy. The aging immune system makes us more susceptible to infections. It explains why even the seasonal flu or COVID-19 can be life-threatening if you are elderly.
Would rejuvenating the immune system with stem cells be the future solution to this problem? Will it be possible to transfuse blood from a younger, healthier donor to boost your grandmother or grandfather’s immune system to extend their life?
References
Simon, AK, Hollander, GA, and McMicheal, A. (2015) Evolution of the immune system in humans from infancy to old age. Proc Biol Sci. Dec 22;282(1821):20143085. Doi: 10.1098/rspb.2014.3085.
Neves, J, Sousa-Victor, P and Jasper, H. (2017) Rejuvenating Strategies for Stem Cell-Based Therapies in Aging. Cell Stem Cell. 2;20(2):161-175. Doi: 10.1016/j.stem.2017.01.008.
Aunan, JR, Watson, MM, Hagland, HR, Søreide, K. (2016) Molecular and biological hallmarks of ageing. Br J Surg. 103(2):e29-46. Doi: 10.1002/bjs.10053.
Related Posts
Novel Cord Blood Stem Cell Treatment Leads to HIV Remission

Stem Cell Transplantation Shows Potential in Stroke Recovery